Reimbursement, revenue, payment, or better yet, the term “cash flow” seems to be on the mind of every home health agency in the nation today. Not only were agencies hit with the RAP reduction from 60% to a minimum 20% with the start of PDGM in January 2020; but the COVID-19 pandemic, which began in March, seemed to throw gasoline onto an already large cash flow fire by increasing the occurrence of LUPAs (Low Utilization Payment Adjustment).
Some of the challenges that agencies seem to struggle with included missed visits and decreased referrals as the public health emergency raged on. Statistics tell us that while CMS predicted a 6-7% LUPA expectancy in PDGM, the nation was actually almost at double that expectancy in October, with a staggering 12.8%.
Question Worth Asking: How can agencies appropriately correct their LUPA problem challenges and optimize their revenue going forward?
HealthPRO Heritage has some advice!
First, agencies need to know up front what their LUPA thresholds are for each 30-day payment period. Agencies know that under PDGM we have what we call a moving LUPA that ranges from two to six visits each 30-day payment period. Upon analysis of the PDGM data and moving LUPA thresholds, we identified that the maximum visit requirement for the first 30 days is six visits, and the maximum visit requirement for the second 30 is three visits. These could be targets to facilitate appropriate care planning across both 30 day payment periods. Studies show that when agencies skill into the second 30-day episode it helps reduce the risk of hospital readmission and facilitates improved patient outcomes and satisfaction.
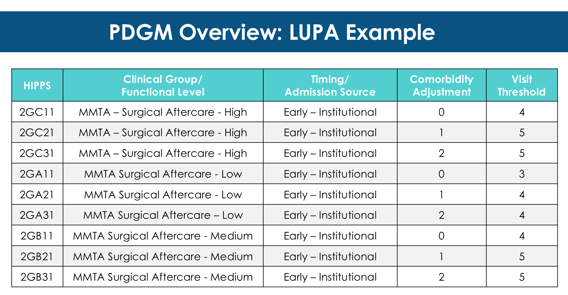
LUPA example of clinical grouping
Second, agencies have an opportunity to improve care planning to maximize clinical outcomes and ensure an appropriate length of stay, which should most times result in care being provided into the 2nd 30 day payment period. National statistics show that the average patient length of stay on home health is around 1.6 payment periods or 47 days. During HealthPRO Heritage’s engagement with many home health agencies, we are finding a trend of LUPA risk in the second 30 day payment period due to poor care planning and care coordination. Of those LUPA trends that have been reviewed, sixty percent of those cases agencies missed the full revenue payment by just one visit. When this is the result of poor care planning and care coordination, there is potentially a loss of around $1,300 in revenue per instance.
It is important to educate clinicians on how a 30-day calendar works and how the second 30-day episode could start in the middle or end of the week for some patients and visits can be scheduled according. Clinicians must be mindful of how the 30 day payment periods work within each 60 day episode of care. Strategic scheduling between different disciplines should be considered as well as staggering when disciplines are involved in a case. Remember, a large % of LUPAs are likely preventable and avoidable under PDGM.
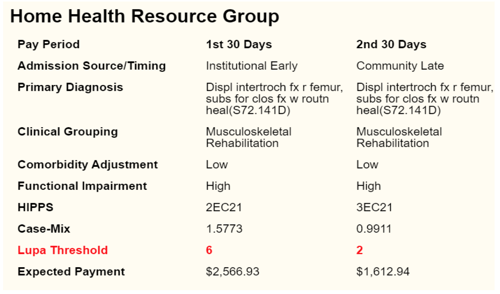 Sample of patient’s clinical data plugged into PDGM Calculator to find out expected payment
Sample of patient’s clinical data plugged into PDGM Calculator to find out expected payment
Third, agencies may have an opportunity to improve both ICD-10 coding and OASIS scoring. Focus on OASIS scoring is imperative at the start of care and discharge. Clinicians need adequate education and training on correctly identifying the appropriate score on the functional independence level M-item questions. These questions not only effect revenue, but also effect quality scores and agency star ratings. Identifying appropriate comorbidities and ensuring the associated ICD-10 codes are on the OASIS can help capture additional revenue that many agencies are leaving on the table. The financial difference can be anywhere between one hundred and three hundred dollars depending on the co-morbidities that are present.
We are here to help. HealthPRO Heritage’s Care Pathways to Success, partnered with our consulting, can assist your agency with future endeavors. Contact us today at homehealth@healthpro-heritage.com and let us help set you up for success in 2021 & beyond!


