It can be easy to get lost in the details of PDGM and forget how vital outcomes and ratings are in driving overall agency success. It’s one of the biggest reasons why appropriately managing therapy in PDGM is a key competency.
In HealthPRO Heritage at Home's recent survey with the National Association for Home Care and Hospice regarding therapy in PDGM, 48% of respondents anticipate less therapy utilization. Agencies should be cautioned on cutting therapy utilization given the focus on functional assessment and outcomes. Functional assessments - completed best by a skilled therapist - will contribute significantly to payment in PDGM, while also continuing to drive publicly reported outcome measures and star ratings.
Achieving positive functional outcomes begins with the right assessment and results in:
- Elevated star ratings - which better positions agencies in narrowing networks;
- Improved patient satisfaction - which enhances HHCAHPS surveys and drives referrals; and
- Enhanced agency scoring in Value Based Purchasing - which CMS plans to make mandatory in every state by 2022.
Functional Scoring in PDGM
Impact on Census Volume
Improvement or decline of these functional measures is a key component of CMS Star Ratings methodology. Remember star ratings are public information available on medicare.gov. Decision makers including patients, families, preferred network administrators, and discharge planners use them in choosing a home health agency.
Recent research shows that home health therapy improves the functional recovery of patients, and lowers risk of re-hospitalization up to 82% contributing greatly to patient satisfaction. Agencies that drastically change use of therapy under PDGM, will see negative outcomes on their quality measures, publicly reported measures, and patient satisfaction scores.
Impact on PDGM Payment Rates
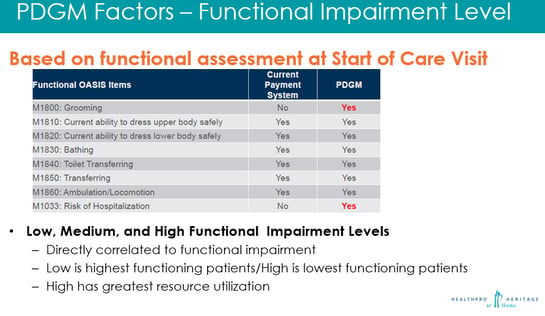
As the table above shows, functional impairment level will be scored using 8 OASIS items. Functional impairment level is one of the 5 direct payment factors in PDGM. The 30-day case mix will in part be determined by low, medium, or high impairment levels which will appropriately indicate the expected use of resources. More resources will be required the higher the impairment level is, thus payment is increased. Accurate assessment is vital.
Impact on VBP Payment Rates
In the current 9 Home Health Value Base Purchasing (HHVBP) states, CMS will adjust payments either negatively or positively based on the quality of care provided as evidenced by patient outcomes. In 2019, the impact is as much as 5% and will grow to be 8% by 2022. Quality of care matters, and therapy has been proven to drive improved outcomes.
The Bottom Line
In PDGM, the importance of functional assessment accuracy is heightened. Ensuring the therapists that treat your patients understand how to accurately assess & document comprehensive clinical needs, care plans, and functional progress will impact your agency’s quality ratings, patient satisfaction, and payment.
Pro-Tip
At HealthPRO Heritage at Home, we are investing in advanced OASIS certification for all our therapy managers and trainers to better support our agency partners in PDGM.
Partnering with the right therapy resource who understands these technical requirements, manages staff to a high standard of quality and timeliness, and who is willing to adapt contractual arrangements to reflect PDGM success drivers, can make all the difference.
To learn more about our approach to PDGM, contact us at homehealth@healthpro-heritage.com
#Ready4PDGM


